
Modelling the projected clinical and Environmental burden of CKD in Egypt and Morocco between 2025 and 2030
This poster, presented at the World Congress of Nephrology 28–31 March 2026 presents work on the clinical and environmental burden of chronic kidney disease (CKD) in Egypt and Morocco between 2025 and 2030. Virtual populations representative of Egypt and Morocco were generated using a microsimulation model. Modelled individuals progressed through CKD stages based on age-related estimated glomerular filtration rate (eGFR) decline rates, and associated comorbidities. Between 2025 and 2030, CKD prevalence was projected to increase substantially in both countries from 5.58m to 7.72m cases in Egypt and from 1.58m to 1.86m in Morocco, with a corresponding significant increase in the environmental impact arising from heamodialysis. Potential responses to mitigate this burden include the implementation of national and regional strategies for early CKD screening and treatment, and integrated approaches to environmental sustainability to mitigate the projected clinical and environmental burden of CKD.

A Population Genetics–Based Microsimulation Platform for Forecasting the Health and Economic Burden of Rare Genetic Diseases
This poster prepared for the World Evidence, Pricing and Access Congress Europe, 2026, Amsterdam (March 3rd-4th 2026), presents HealthLumen's work on modelling the health and economic burden of rare genetic diseases. Microsimulation allows individual-level modelling based on population demographics, ancestry-linked genetic data, disease penetrance data, and other relevant parameters. Integration of such datasets allows the model to overcome data scarcity in other areas, e.g. national prevalence estimates, which is a key challenge in rare diseases. The model can be leveraged to generate evidence to raise awareness of disease burden and effective interventions, and inform payers, providers and policymakers to advance access to timely and effective treatment for rare disease patients.

Quantifying the proportion of women at risk of an FNAIT pregnancy in diverse populations in the United States
This poster, presented at the 2024 American Society of Human Genetics Meeting, November 5–9 (Denver, CO), details the first study to report FNAIT risk across diverse ancestries using data from genetic databases to calculate the expected number of women carrying underlying causal genetic variants. The study suggests that nearly 20,000 pregnancies in the US are at higher FNAIT risk each year – a significantly greater number than previously estimated – and supports the case for screening all pregnant women for potential FNAIT risk, regardless of race and ethnicity.

Estimating the Prevalence of Late-Onset Fabry Disease in the United States in 2024
This poster, prepared for the World Orphan Drug Congress Europe 2024, Barcelona (October 23–25, 2024), presents HealthLumen's work on estimating the prevalence of late-onset Fabry disease in the US in 2024 by analysing selected GLA variants mostly associated with late-onset Fabry disease, projecting their allele frequencies to the US population, and applying penetrance data to determine the number of symptomatic carriers. The carrier and symptomatic populations of Fabry disease in the US in 2024 according to the 8 variants included for analysis in this study are: 24,845 female carriers, of whom 17,392 will develop symptoms, and 12,024 male carriers, all of whom will develop symptoms.

Pragmatic literature reviews to populate a patient-level model and project the future economic burden of CKD in low-and middle-income countries
This poster, presented at the 61st European Renal Association Congress in Stockholm, Sweden (May 23–26, 2024), outlines how pragmatic literature reviews were conducted to populate a patient-level microsimulation model used to project the future economic burden of chronic kidney disease (CKD) in low- and middle-income countries from 2024–2029. Country-specific data collected included country demographics, disease prevalence data for CKD, kidney replacement therapies (KRTs), comorbidities and cardiovascular complications. For the health economics module, annual per-patient direct healthcare costs and disability weights associated with treating CKD, undergoing KRTs, and managing complications were included. Proxy data was used where country-specific data was limited. The results of the microsimulation estimated that by 2029, CKD costs (including KRT) were projected to reach $47.8M in Kenya, and $219.0M in Uzbekistan, of which $29.5M and $72.9M were for KRTs respectively. Such microsimulation modelling can help to estimate the economic benefits that could be achieved in low- and middle-income countries through national policies aiming to reduce CKD burden – including earlier diagnosis and treatment to slow disease progression.
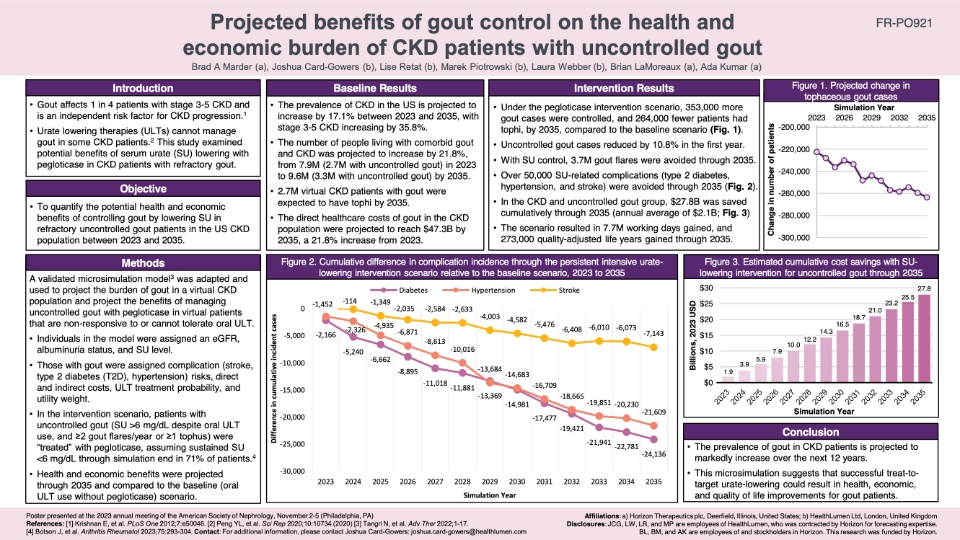
Projected benefits of gout control on the health and economic burden of CKD patients with uncontrolled gout
This poster, presented at the annual meeting of the American Society of Nephrology in Philadelphia, USA (November, 2023) outlines the findings of a study examining the potential benefits of serum urate (SU) lowering using pegloticase in chronic kidney disease (CKD) patients with refractory gout. The study, using microsimulation modelling, found that under a pegloticase intervention scenario, 353,000 more gout cases were controlled, and 264,000 fewer patients had tophi, by 2035, compared to the baseline scenario. Further, the SU lowering intervention was projected to save $27.8B, and gain 7.7M working days, cumulatively through 2035. This study consequently provides evidence that successful treat-to-target urate-lowering could result in health, economic, and quality of life improvements for gout patients.

Inside CKD: Projecting the Population Level Clinical Burden of Chronic Kidney Disease According to Urine Albumin-to-Creatine Ratio (uACR) Categories
This study assessed the future epidemiological and financial burden of CKD using the Inside CKD microsimulation. Specifically, it reports on the CKD population level projections for cardio-renal complications, progression to end stage kidney disease (ESKD), and death due to any cause according to uACR categories.
The results support early intervention in the total CKD population, including individuals with normo- or micro-albuminuria, to reduce cardio-renal outcomes, delay progression to ESKD, and therefore avoid the requirement for costly interventions, including heart related hospitalisations, transplantation and dialysis.

HepaHealth II: Preventing liver disease with policy measures to tackle alcohol consumption and obesity
Chronic liver disease (CLD) causes 1.8% of all deaths in Europe. Without policies to mitigate harmful alcohol consumption and obesity, that proportion will continue to increase. This major study, commissioned by EASL and supported by an unrestricted education grant from Bristol-Myers Squibb and Gilead, was carried out over the past 3 years and estimates the impact of policy interventions targeting alcohol and obesity on the incidence of CLD and primary liver cancer in France, the Netherlands, and Romania. The project builds on our previous work published in 2018.
Our peer-reviewed microsimulation model was employed to project trends in alcohol consumption and body mass index (BMI) from 2022 to 2030. We modelled the incidence of CLD and liver cancer under three policy scenarios versus an inaction scenario. All policies had an important impact ranging from a 2% to 7% reduction in annual incidence of CLD and liver cancer by 2030. The most effective scenarios are an increased Minimum Unit Pricing (MUP) of €1 on alcohol or introducing a set of complementary public health policies targeting an increased MUP, a sugar sweetened beverage (SSB) tax, and a volumetric tax that target both alcohol consumption and obesity.
View the poster presented at the EASL Congress in Vienna (June 2023)
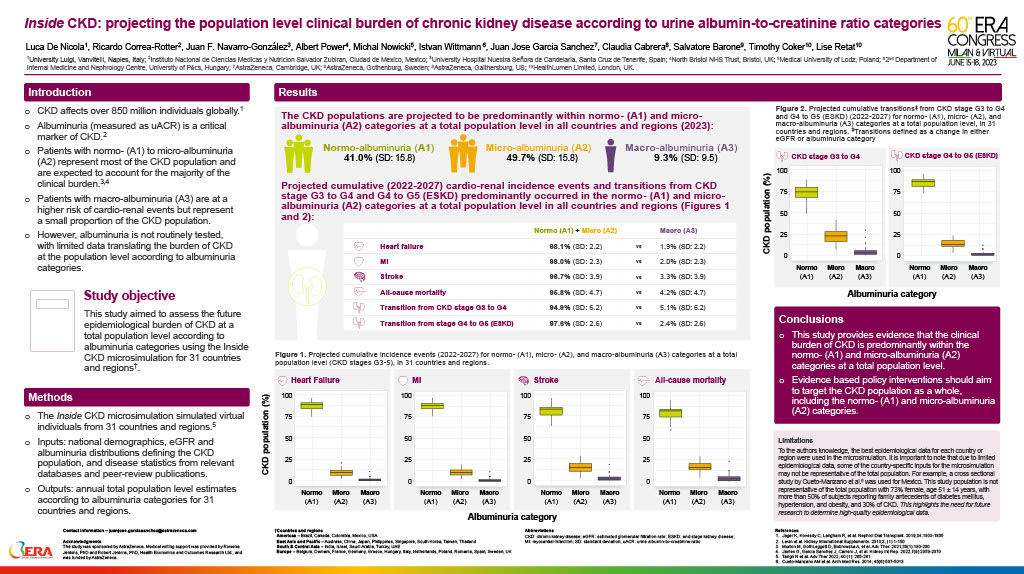
Inside CKD: projecting the population level clinical burden of chronic kidney disease according to urine albumin-to-creatinine ratio categories
This poster, presented at the European Renal Association’s 60th Congress in Milan (June 2023), summarises research on projecting the population level clinical burden of Chronic Kidney Disease (CKD) according to urine albumin-to-creatinine ratio categories. The study provides evidence that the clinical burden of CKD is predominantly within the normo-(A1) and micro-albuminuria (A2) categories at a total population level. Evidence based policy interventions should aim to target the CKD population as a whole, including the normo-(A1) and micro-albuminuria (A2) categories.
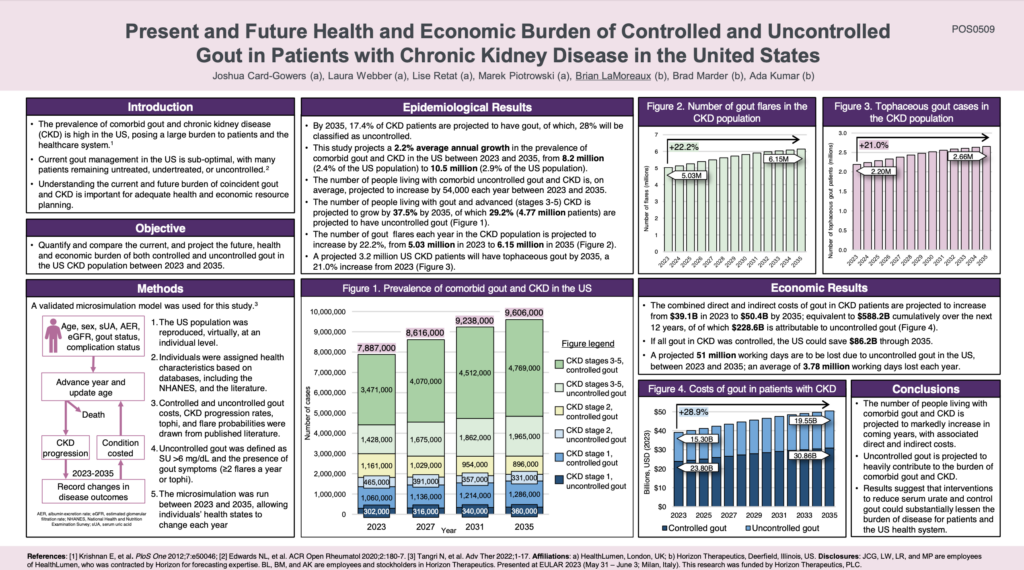
The Present and Future Health and Economic Burden of Controlled and Uncontrolled Gout in Patients with CKD in the US
This poster, presented at EULAR 2023, showcases our new research that projects the increasing health and economic burden of comorbid gout and CKD, in the US, between 2023 and 2035. This study is the first to project the burden of comorbid gout and CKD and highlights the need for strategies that can effectively control gout in CKD patients.