
HepaHealth II: Preventing liver disease with policy measures to tackle alcohol consumption and obesity
Chronic liver disease (CLD) causes 1.8% of all deaths in Europe. Without policies to mitigate harmful alcohol consumption and obesity, that proportion will continue to increase. This major study, commissioned by EASL and supported by an unrestricted education grant from Bristol-Myers Squibb and Gilead, was carried out over the past 3 years and estimates the impact of policy interventions targeting alcohol and obesity on the incidence of CLD and primary liver cancer in France, the Netherlands, and Romania. The project builds on our previous work published in 2018.
Our peer-reviewed microsimulation model was employed to project trends in alcohol consumption and body mass index (BMI) from 2022 to 2030. We modelled the incidence of CLD and liver cancer under three policy scenarios versus an inaction scenario. All policies had an important impact ranging from a 2% to 7% reduction in annual incidence of CLD and liver cancer by 2030. The most effective scenarios are an increased Minimum Unit Pricing (MUP) of €1 on alcohol or introducing a set of complementary public health policies targeting an increased MUP, a sugar sweetened beverage (SSB) tax, and a volumetric tax that target both alcohol consumption and obesity.
View the poster presented at the EASL Congress in Vienna (June 2023)
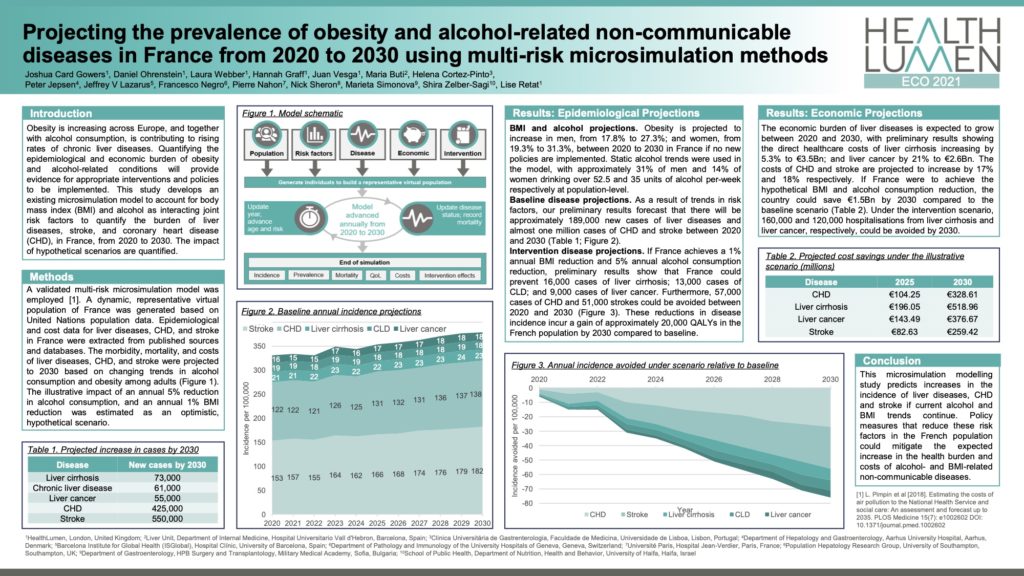
The burden of liver diseases, stroke, and coronary heart disease in France, to 2030
Obesity is increasing across Europe, and together with alcohol consumption, is contributing to rising rates of chronic liver diseases. Quantifying the epidemiological and economic burden of obesity and alcohol-related conditions will provide evidence for appropriate interventions and policies to be implemented. This study develops an existing microsimulation model to account for body mass index(BMI) and alcohol as interacting joint risk factors to quantify the burden of liver diseases, stroke, and coronary heart disease(CHD), in France, from 2020 to 2030. The impact of hypothetical scenarios are quantified.
View overview video

Tipping the scales: Why preventing obesity makes economic sense
Together with Cancer Research UK, we produced a report which looked at the health and economic impact of ever-increasing overweight and obesity rates in the UK. We showed that even a small reduction in obesity prevalence could offset the significant health and economic cost of doing nothing.

REBALANCE: Mixed-methods systematic review and economic evaluation for severe obesity
A study to systematically review bariatric surgery, weight-management programmes (WMPs) and orlistat pharmacotherapy for adults with severe obesity, and evaluate the feasibility, acceptability, clinical effectiveness and cost-effectiveness of treatment.

Obesity in primary care: Screening and brief intervention
The Brief Intervention for Weight Loss Trial enrolled consecutively attending primary care patients who were obese and participants were randomised to physicians opportunistically endorsing, offering, and facilitating a referral to a weight loss programme (support) or recommending weight loss (advice). We use a cohort simulation to predict effects on disease incidence, quality of life, and healthcare costs over 20 years.

Inequalities in smoking and obesity in Europe predicted to 2050
This study projected educational inequalities in obesity and smoking prevalence to 2050 based on past obesity and smoking trends by education level. The conclusion was that widening educational inequalities in obesity and smoking prevalence are expected in several European countries if current trends in obesity and smoking prevalence are unaltered. This will impact on inequalities in morbidity and mortality of associated diseases such as diabetes, coronary heart disease and chronic obstructive pulmonary disease.

Forecasting Future Trends in Obesity across Europe: The Value of Improving Surveillance
This project projected the prevalence of obesity across the WHO European region and examined whether the WHO target of halting obesity at 2010 levels by 2025 is achievable. The results were that by 2025, obesity is projected to increase in 44 countries. If present trends continue, 33 of the 53 countries are projected to have an obesity prevalence of 20% or more.

High Rates of Obesity and Non-Communicable Diseases Predicted across Latin America
Non-communicable diseases (NCDs) such as cardiovascular disease and stroke are a major public health concern across Latin America. We used our microsimulation model to project BMI and related disease trends to 2050. We tested the extent to which interventions that decrease body mass index (BMI) have an effect upon the number of incidence cases avoided for each disease. Without intervention obesity trends will continue to rise across much of Latin America.

Alarming predictions for obesity and non-communicable diseases in the Middle East
This study used our microsimulation model to project obesity trends and future obesity-related disease for nine countries in the Middle East. We found that high rates of overweight and obesity increased in both men and women in most countries. Obesity is a growing problem in the Middle East which requires government action on the primary prevention of obesity.

F as in Fat: How obesity threatens America’s future
In this report we modelled the long-term health impacts of obesity in each US state. The results were used as part of an annual report produced by Trust for America’s Health and sponsored by Robert Woods Johnson Foundation.